
Continuity and Clinical Excellence in Multinational Healthcare Teams
Continuity and Clinical Excellence in Multinational Healthcare Teams
While clinical and technical alignment is a given in any healthcare team, patient safety and treatment precision ultimately depend upon shared cultural and communication norms.
Without this common cohesion on norms and operational culture, even the most clinically proficient teams risk falling out of sync, thereby amplifying systemic risks as well as increasing the risk for patients
The Strategic Value of Cross-National Collaboration in Medicine and Health Care
1. Securing Critical Clinical Expertise
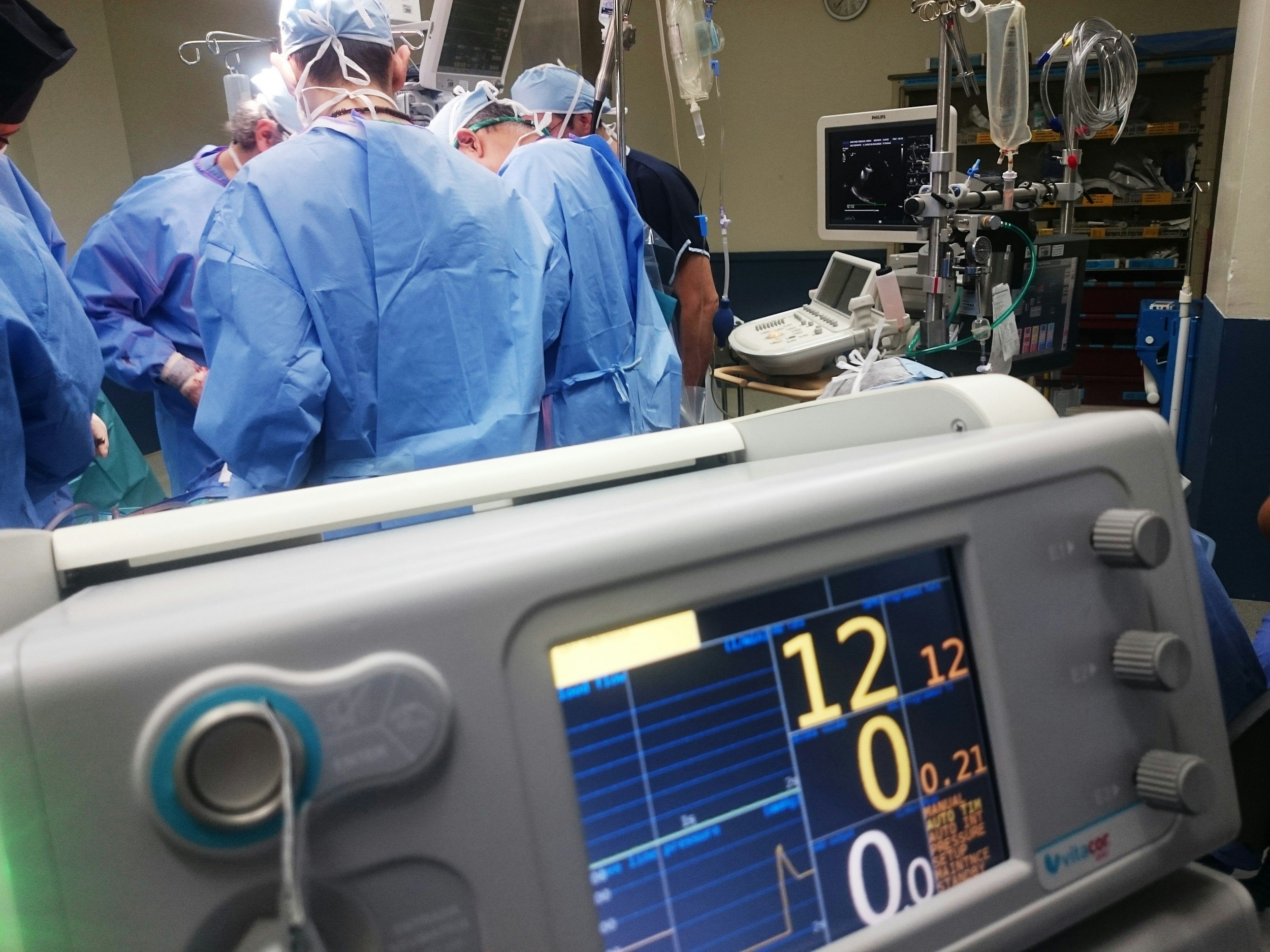
Recruiting top-tier international medical expertise is a substantial strategic investment. Yet, technical proficiency alone does not guarantee effective collaboration. If a highly trained specialist resigns after merely six months due to cultural friction and poor integration with the operational model, the department—and potentially the broader regional healthcare provision—suffers a severe structural loss.
2. Enhancing Treatment Quality Through Cohesive Collaboration

Newly appointed international staff frequently encounter operational paradigms that feel alien compared to their prior experiences, as different nations inherently possess distinct working methodologies. By cultivating expertise in multinational management within these teams, healthcare institutions can bridge these cognitive silos, securing both the stability of the workforce and the fundamental safety of clinical services.
3. Empowering Healthcare Leaders to Builds Safer Environments
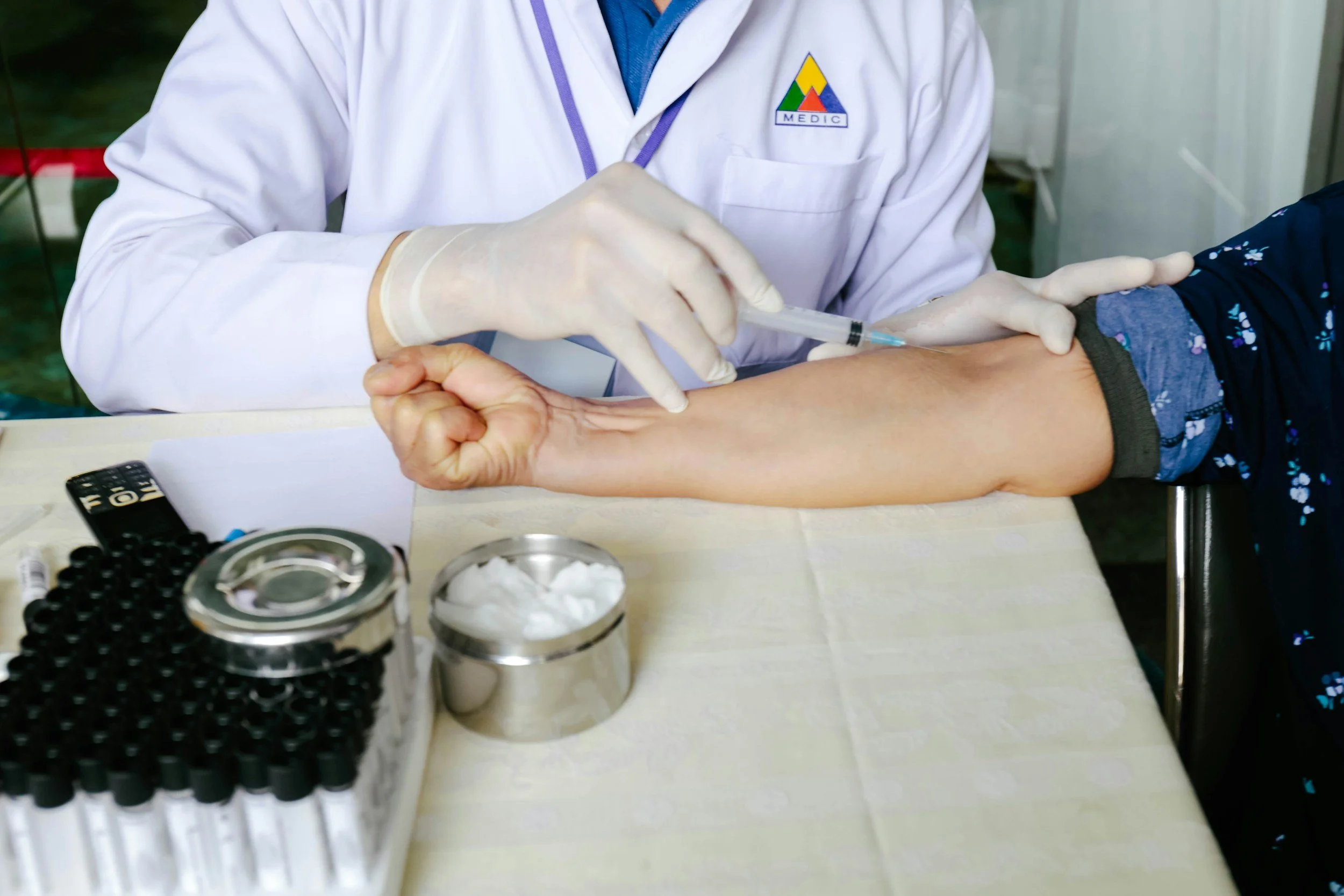
Regulatory and institutional demands regarding the psychosocial working environment are increasingly more valued, encompassing clear role definition, structural support, staff participation, and dignity for all personnel. For international healthcare professionals, it is particularly vital to address ambiguous expectations, unfamiliar communication norms, and a lack of grounding in domestic workplace culture. Expertise in multinational leadership is therefore a structural prerequisite to ensuring a fully defensible, compliant, and safe working environment for all staff, irrespective of their cultural origins.
“Research indicates that teams where one in four nurses is internationally educated frequently experience communication breakdowns and elevated frustration. A national study from New Zealand - a country with working norms highly analogous to our own, revealed drastically divergent expectations regarding hierarchy and the distribution of responsibility within healthcare teams. The study further illuminated that such disparities in working and communication norms, particularly concerning role comprehension, made it profoundly challenging for teams to navigate periods of uncertainty in a cohesive, structured manner.”
Healthcare Knowledge and Leadership —
From the Inside Out
Effective healthcare leadership begins with knowing what it actually feels like on the floor. The pace of a busy A&E. The precision behind a surgical unit. The quiet resilience of the people who hold it all together when the pressure peaks.
Over more than ten years, I led teams at one of Norway’s largest research hospitals — working across orthopaedics, acute and emergency care, oncology, pulmonology, and most inpatient and outpatient settings.
That lived experience is an integral part of what I bring to multinational healthcare teams and leadership development.
